2 results
An Observational Study on CRE Colonization and Subsequent Risk of Infection in Adult ICU Patients
- Kirtika Sharma, Vibhor Tak, Vijaya Lakshmi Nag
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, pp. s66-s67
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Carbapenem-resistant Enterobactericeae (CRE) has emerged as a global health threat with increasing incidence. It is a particular problem in India because control over antibiotics prescription is really poor; these agents can be easily bought over the counter and the antibiotic prescription threshold is low among Indian doctors. Also, even when administered, antibiotics are given in inappropriate dosages and durations. CRE infections are a healthcare challenge due to their difficulty to treat and high morbidity and mortality. Colonization requires infection prevention measures, and it should be prioritized. Methods: We sought to determine the prevalence rate of CRE colonization in the gastrointestinal tract in newly admitted ICU patients along with follow-up of any subsequent infection following colonization. A prospective observational study was carried out among ICU patients from January 2019 to August 2020 by collecting perirectal swabs from patients who gave consent. Clinical variables were identified, and the relationship between CRE colonization and subsequent systemic CRE infection was assessed. Processing was carried out by culturing on MacConkey agar plate with ertapenem disk and further identified using conventional microbiological techniques. The ertapenem MIC was determined using an Epsillometer (E) test. The modified carbapenem inactivation (mCIM) test and the EDTA carbapenem inactivation method (eCIM) were used to confirm carbapenem resistance using Clinical Laboratory Standards Institute 2020 guidelines (Figure 1). Results: Among 192 ICU patients, 37 (19.27%) were colonized with CRE (Table 1). Also, 13 (35.13%) CRE isolates showed metallo-β-lactamase resistance. Furthermore, 18 CRE isolates (48.64%) showed serine carbapenemase activity; 6 CRE isolates showed no carbapenemase activity. Klebsiella pneumoniae (n = 25 of 37, 67.56%) was the most common CRE isolated followed by Escherichia coli (n = 11 of 37, 29.72%) and 1 isolate of Enterobacter spp (n = 1 of 37, 0.02%). Of 37 patients, 33 (89.18%) developed CRE infection during their hospital stay. Pneumonia was the most common infection developed (36.36%), followed by surgical site infection (21.21%) and urinary tract infection (12.12%). Only 1 patient developed a bloodstream infection. However, 9 patients (27.27%) developed multiple-site infections. Of 37 CRE-colonized patients, 10 (27.02%) died during their hospital stay. Conclusions: Our study highlights the increased risk of CRE infection and mortality in patients with CRE colonization in ICU patients. Hence, CRE perirectal screening for detection of asymptomatic carriers should be conducted, and strict infection control measures, such as isolation and cohorting with barrier nursing of such patients, should be done to prevent further spread of CREs in hospital settings.
Funding: No
Disclosures: None
Figure 1.
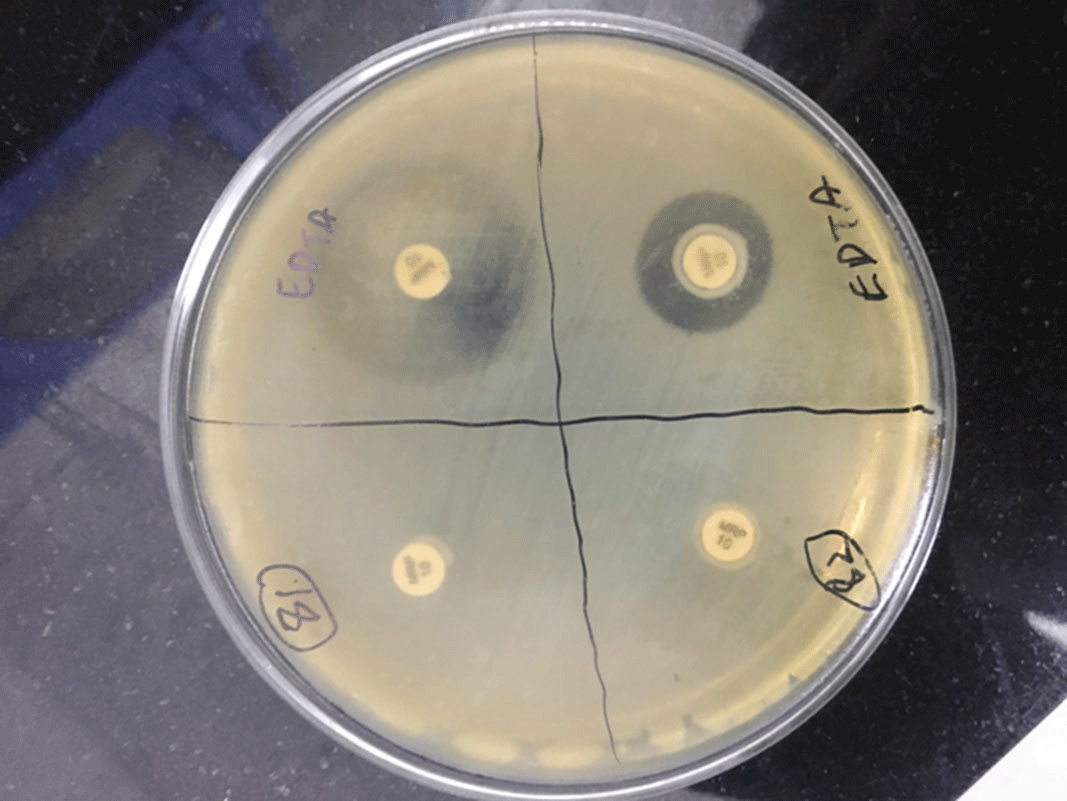
Table 1. 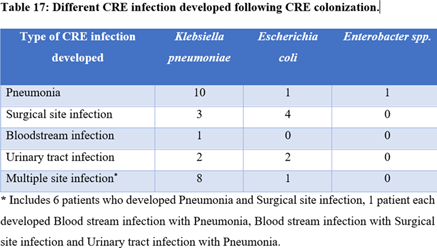
Table 2. 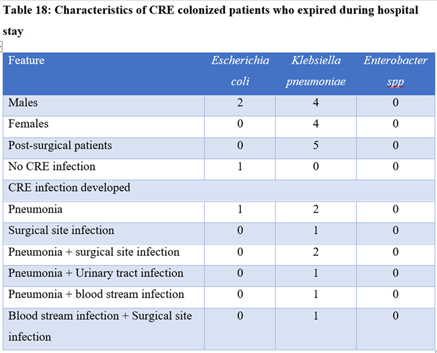
Surveillance of Healthcare-Associated Bloodstream and Urinary Tract Infections in a National Level Network of Indian Hospitals
- Purva Mathur, Paul Malpiedi, Kamini Walia, Rajesh Malhotra, Padmini Srikantiah, Omika Katoch, Sonal Katyal, Surbhi Khurana, Mahesh Chandra Misra, Sunil Gupta, Subodh Kumar, Sushma Sagar, Naveet Vig, Pramod Garg, Arti Kapil, Manoj Sahu, Arunaloke Chakrabarti, Pallab Ray, Manisha Biswal, Neelam Taneja, Priscilla Rupali, Vellore Binila Chacko, Joy Sarojini Michael, Veeraraghavan Balaji, Camilla Rodrigues, Vijaya Lakshmi Nag, Vibhor Tak, Vimala Venkatesh, Chiranjay Mukhopadhyay, KE Vandana, Muralidhar Varma, Vijayshri Deotale, Ruchita Attal, Kanne Padmaja, Chand Wattal, Neeraj Goel, Sanjay Bhattacharya, Tadepalli Karuna, Saurabh Saigal, Bijayini Behera, Sanjeev Singh, MA Thirunarayan, Reema Nath, Raja Ray, Sujata Baveja, Mammen Chandy, Sudipta Mukherjee, Manas Roy, Gaurav Goel, Swagata Tripathy, Satyajeet Misra, Anupam Dey, Tushar Mishra, Hirak Raj, Bashir Fomda, Gulnaz Bashir, Shaista Nazir, Sulochana Devi, Khuraijam Ranjana Devi, Langpoklakpam Chaoba Singh, Padma Das, Anudita Bhargava, Ujjwala Gaikwad, Neeta Khandelwal, Geeta Vaghela, Tanvi Sukharamwala, Prachi Verma, Mamta Lamba, Shristi Jain, Prithwis Bhattacharyya, Anil Phukan, Clarissa Lyngdoh, Rajeev Sharma, Rajni Gaind, Rushika Saksena, Lata Kapoor, Neil Gupta, Aditya Sharma, Daniel VanderEnde, Anoop Velayudhan, Valan Siromany, Kayla Laserson, Randeep Guleria
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s398-s399
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Healthcare-associated infections (HAIs) are a major global threat to patient safety. Systematic surveillance is crucial for understanding HAI rates and antimicrobial resistance trends and to guide infection prevention and control (IPC) activities based on local epidemiology. In India, no standardized national HAI surveillance system was in place before 2017. Methods: Public and private hospitals from across 21 states in India were recruited to participate in an HAI surveillance network. Baseline assessments followed by trainings ensured that basic microbiology and IPC implementation capacity existed at all sites. Standardized surveillance protocols for central-line–associated bloodstream infections (CLABSIs) and catheter-associated urinary tract infections (CAUTIs) were modified from the NHSN for the Indian context. IPC nurses were trained to implement surveillance protocols. Data were reported through a locally developed web portal. Standardized external data quality checks were performed to assure data quality. Results: Between May 2017 and April 2019, 109 ICUs from 37 hospitals (29 public and 8 private) enrolled in the network, of which 33 were teaching hospitals with >500 beds. The network recorded 679,109 patient days, 212,081 central-line days, and 387,092 urinary catheter days. Overall, 4,301 bloodstream infection (BSI) events and 1,402 urinary tract infection (UTI) events were reported. The network CLABSI rate was 9.4 per 1,000 central-line days and the CAUTI rate was 3.4 per 1,000 catheter days. The central-line utilization ratio was 0.31 and the urinary catheter utilization ratio was 0.57. Moreover, 3,542 (73%) of 4,742 pathogens reported from BSIs and 868 (53%) of 1,644 pathogens reported from UTIs were gram negative. Also, 1,680 (26.3%) of all 6,386 pathogens reported were Enterobacteriaceae. Of 1,486 Enterobacteriaceae with complete antibiotic susceptibility testing data reported, 832 (57%) were carbapenem resistant. Of 951 Enterobacteriaceae subjected to colistin broth microdilution testing, 62 (7%) were colistin resistant. The surveillance platform identified 2 separate hospital-level HAI outbreaks; one caused by colistin-resistant K. pneumoniae and another due to Burkholderia cepacia. Phased expansion of surveillance to additional hospitals continues. Conclusions: HAI surveillance was successfully implemented across a national network of diverse hospitals using modified NHSN protocols. Surveillance data are being used to understand HAI burden and trends at the facility and national levels, to inform public policy, and to direct efforts to implement effective hospital IPC activities. This network approach to HAI surveillance may provide lessons to other countries or contexts with limited surveillance capacity.
Funding: None
Disclosures: None






